The Green Clinic – behoefte aan goede gezondheidszorg
Jan. 2017 | This post describes the need for a Health Care and Prevention Clinic from a ‘bottom-up’ point of view. What is the problem exactly at community level and to what extent do other stakeholders at district and national policy level regard this as problem as well? This determines the institutional support that is available and offers input for a possible solution that will be designed at community level.
Point of view at Community Level
The community members almost unanimously affirmed that the lack of a health care facility in the community is their main challenge. They referred to the struggle pregnant women go through before they reach the hospital. The nearest hospital is Bator Catholic Hospital and one needs to cross the river by canoe in order to reach there. For medical advice on minor ailments they have to undertake the same journey and spend almost a full day before a doctor or nurse attends to them. Consequently, going to chemical store or using traditional medicine to cure their illnesses without seeking medical advice is much easier and therefore common practice.
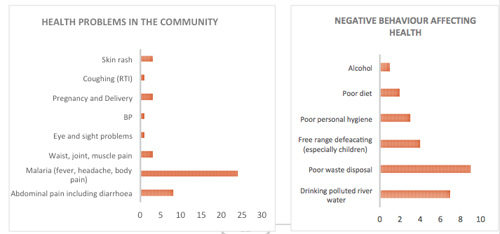
Secondly, they are aware of behavior that causes health problems and diseases that could be prevented. However, there is no health facility and no health educational programs are conducted, apart from weighing and vaccination of children in the neighboring community. The outcome of the community health survey among 30 community members explained that the perceived health problems could often be taken care of at primary health care level. It also shows that the people know that they practice unfavorable behavior but are not equipped with either knowledge or infrastructure to change this.
The two graphs below show some results of the community health survey. It shows the health problems people experience and the unfavorable behavior practiced.
Point of view at District Level
Representatives of the following institutions where interviewed on health issues in the districts and on the feasibility of a health facility in Atsiekpoe:
- Bator Catholic Hospital (Secondary)
- Volo Governmental Health Clinic (Primary)
- North-Tongu Health Directorate
- North-Tongu District Assembly
Full abstracts of these interviews are available on request, but the most important relevant information is written below.
Bator Catholic Hospital is a well-known medical facility that is part of the National Catholic Health Services (NCHS). The NCHS together with other faith based hospitals fall under CHAC which is part of the Ministry of Health (MoH). The hospital offers general medical services, however their specialization is still surgery and gynecology. Advanced technology is available such as colposcopy to detect and treat cervical cancer. Furthermore, they have a maternal and child health department, and offer mental and reproductive health (including HIV/AIDS) services. One of the challenges they experience are the large number of people with minor ailments who come to the hospital but who ideally should be seen at primary health care level. As a secondary institution, they prefer focusing on their specialization and to attend to patients who are referred for special care. Data on the most common diseases diagnosed in the hospital are not applicable to a riverbank community like Atsiekpoe as the hospital receives patients from a much wider geographical area, like Greater Accra and Volta Region.
 Volo Health Centre is a primary health clinic where people from Atsiekpoe also go to seek medical advice. The Health Centre is a Class M clinic, which means that the clinic is headed by a midwife. Other staff members are four community health nurses and a health assistant. Class M classification means that maternal health services are the main services offered, however they also run a general clinic and offer reproductive and child health services. Critical cases are referred to Bator Hospital and these are often severe malaria patients who waited too long before seeking medical help.
Volo Health Centre is a primary health clinic where people from Atsiekpoe also go to seek medical advice. The Health Centre is a Class M clinic, which means that the clinic is headed by a midwife. Other staff members are four community health nurses and a health assistant. Class M classification means that maternal health services are the main services offered, however they also run a general clinic and offer reproductive and child health services. Critical cases are referred to Bator Hospital and these are often severe malaria patients who waited too long before seeking medical help.
The diseases seen in the clinic have a very strong correlation with the geographic factors of the riverbank communities. The overview of main diseases seen at Volo Health Centre represent the situation in the riverbank communities in the district. The main diseases are:
- Diarrhea
- Malaria
- Skin Infections
- Urinal Tract infections
Waterborne diseases (like Bilharzia) from polluted drinking and bathing water or common underlying causes.
The mandate of the District Health Directorate (DHD) is planning and supervision of health care delivery in the district and translating national policies in the catchment areas. According to the director, the main challenge in the district is health care accessibility. Bridging the equity gap in geographic access to health services is one of their main objectives. Other objectives are related to service delivery, promoting healthy lifestyle, good governance and data management.

Concerning the accessibility to health care, the director affirms that people have to travel long distances to reach a clinic or hospital. On top of that, financial accessibility of health care is also a problem and this was also frequently mentioned by the people in Atsiekpoe. Another main problem affecting the rural communities are the lack of transport means for the community health workers to do outreach work to remote and deprived areas. Since the DHD mainly focusses on translating national policies to the district level, there are no objectives specifically focusing on the health situation in riverbank communities. However, diseases like malaria and upper-tract chest infections, together with high blood pressure and to life style related disorders, are very prevalent and containment is high on the agenda of every DHD. Furthermore, the director stated that the raising number of teenage pregnancies is alarming and requires attention.
Point of view at (Inter)National Level
In the past decennia, the health delivery system in Ghana and other African countries very much evolved based on the direction given by international organizations such as the World Health Organization (WHO) and other UN agencies. Back in 1978, the Alma-Ata Declaration emerged as a milestone one twentieth century in the field of public health, and it identified Primary Health Care (PHC) as the key to the attainment of the WHO’s goal of Health for All.
 PHC was expected to form an integral part of both the countries health system and the overall social and economic development of the community. It would be the first level of contact of individuals, the family and the community to the national health care system bringing health care as close to where people live and work and constitute the first element of a continuing health care process. Improving primary health care was also central to the Millennium Development Goals (MDG), a series of time-bound targets adopted by largest gathering of world leaders during the Millennium Summit in September 2000.
PHC was expected to form an integral part of both the countries health system and the overall social and economic development of the community. It would be the first level of contact of individuals, the family and the community to the national health care system bringing health care as close to where people live and work and constitute the first element of a continuing health care process. Improving primary health care was also central to the Millennium Development Goals (MDG), a series of time-bound targets adopted by largest gathering of world leaders during the Millennium Summit in September 2000.
Since the Alma-Ata declaration, Ghana’s health delivery system focused on expansion on primary health care and health system strengthening, as well as the MDG. However, the endeavors in many African countries have been challenged by complex scenarios such as rapid urbanization, emerge and re-emerge of communicable and non-communicable diseases, and a decline in national economic performance combined with a high depth burden and deterioration of trade. Ghana is no exception, even though it does better on health indicators compared to its neighbors. The objectives of Ghana’s PHC to achieve basic and primary health care for 80% of the people and to effectively deal with the disease problems that contribute to 80% of morbidity and mortality has far from reached.
The strategies for the PHC are still on improving quality, accessibility and coverage of services and to support the primary level of health care service provision. Provision of smaller primary health care infrastructure that are closer to the majority of the people is emphasized.
Conclusion
The main challenge people in Atsiekpoe experience, namely poor accessibility to a primary health care, is the ‘real-life situation’ vigorously spoken about on (inter)national conferences and symposia and written about in (inter)national health care strategies and reports. Access to primary health care is a real problem and tackling this issue at community level is a very laudable idea.
Please visit our fundraising pages
The foundation of the building has been laid out, so now we need the funds to build walls and a roof! We currently have 2 fundraising pages:
Visit our fundraising page on Fundrazr.com to help us finish the building of the clinic.
More info
Laatste nieuws
- Update Liati Wote plastic recycling project en de Green Hub, maart 2022
- Update Liati Wote plastic recycling program March 2020
- Liati Wote community development – Report 6: Creating Awareness Using Wall Paintings
- Liati Wote community development – Report 5: Mounting the segregations waste bins
- A new board member, Chief Sanitation and Development and great help with our plastic waste project
- Liati Wote community development – Report 4: Introduction of the plastic recycling project
- Building The Green Clinic – update february 2019
- Building The Green Clinic – update january 2019
- Building The Green Clinic – update december 2018
- Building The Green Clinic – update november 2018
- Building The Green Clinic – update july 2018
- Building The Green Clinic – update may 2018